LOW COST Shoulder Replacement Surgery in India
LOW COST Shoulder Replacement Surgery in India
Planning Your MedicaTrip to India?
Joint Replacement Surgery Hospital India makes it simple:
- Fill in our enquiry form — our executive will contact you shortly.
- Call us anytime: +91-9860432255
- Complete surgery details are available on our website.
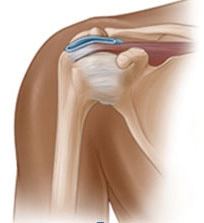
What is Shoulder replacement Surgery?
Shoulder replacementis a surgical procedure in which all or part of the glenohumeral
joint is replaced by a prosthetic implant. Such joint replacement surgery generally is conducted to relieve arthritis pain or fix severe physical joint damage.
Shoulder replacement surgery is an option for treatment of severe arthritis of the shoulder joint. Arthritis is a condition that affects the cartilage of the joints. As the cartilage lining wears away, the protective lining between the bones is lost. When this happens, painful bone-on-bone arthritis develops. Severe shoulder arthritis is quite painful, and can cause restriction of motion. While this may be tolerated with some
medications and lifestyle adjustments, there may come a time when surgical treatment is necessary.
Symptoms-
Patients with arthritis typically describe a deep ache within the shoulder joint. Initially, the pain feels worse with movement and activity, and eases with rest. As the arthritis progresses, the pain may occur even when you rest. By the time a patient sees a physician for the shoulder pain, he or she often has pain at night. This pain may be severe enough to prevent a good night’s sleep. The patient’s shoulder may make grinding or grating noises when moved. Or the shoulder may catch, grab, clunk or lock up. Over time, the patient may notice loss of motion and/or weakness in the affected shoulder. Simple daily activities like reaching into a cupboard, dressing, toileting and washing the opposite armpit may become increasingly difficult.
Common Symptoms of Shoulder Arthritis include:
- Pain with activities
- Limited range of motion
- Stiffness of the shoulder
- Swelling of the joint
- Tenderness around the joint
- A feeling of grinding or catching within the joint
VIDEO – SHOULDER REPLACEMENT SURGERY IN INDIA
Patient Review – African Patient share Success Stories
of Low Cost Shoulder Replacement Surgery in India
Hello, I am Andre Jacobs from South Africa. I got my shoulder replacement surgery in India through Joint Replacement Hospital India. I had experienced soreness in my left shoulder while lifting weights and working in my yard. Over time, this discomfort progressed into pain and started interfering with my daily activities. Though I underwent the physical therapy and took medications, but nothing seemed to work out. It was then, that a friend of my relative who is doctor suggested me about your surgery group in India. I went online searching for more information and impressed with it, I send my inquiry. They called me back and replied to all my queries. They explained me well about the surgery and what I should expect with it. They also asked me for my medical reports and after getting the best treatment options, I got my surgery fixed with them. I had one of the amazing experiences during my trip in India. The surgeon took his time clearing all my doubts and putting me at ease. The whole staff was friendly. Thank you for the wonderful care and quality of service you guys rendered throughout my stay in India.
Shoulder Treatment Options-
Nonsurgical Treatment-
Treatment of an arthritic shoulder starts with rest, exercise and taking arthritis medications. Resting the shoulder and applying moist heat can ease mild pain. After strenuous activity, an ice pack may be more effective at decreasing pain and swelling.
Physical therapy may be helpful when arthritis is in early stages. It helps maintain joint motion and strengthen the shoulder muscles. Physical therapy is less effective when the arthritis has advanced to the point that bone rubs on bone. When this is the case, physical therapy may make the shoulder hurt more.
Arthritis medications, called nonsteroidal anti-inflammatories (NSAIDs), can control arthritis pain. Certain NSAIDs may be purchased over-the-counter, while others require a prescription. Periodic cortisone injections into the shoulder joint can provide temporary pain relief. Excessive cortisone shots can have adverse effects, however.
Surgical Treatment-
If nonoperative treatments fail, shoulder replacement surgery may be needed. Shoulder replacements are usually done to relieve pain.
There are several different types of shoulder replacements. The usual total shoulder replacement involves replacing the arthritic joint surfaces with a highly polished metal ball attached to a stem, and a plastic socket. The components come in various sizes. If the bone is of good quality, your surgeon may choose to use a non-cemented or press-fit humeral component. If the bone is soft, the humeral component may be implanted with bone cement. In most cases, an all-plastic glenoid component is implanted with bone cement. Implantation of a glenoid component is not advised if:
- The glenoid has good cartilage.
- The glenoid bone is severely deficient.
- The rotator cuff tendons are irreparably torn.
Patients with bone-on-bone osteoarthritis and intact rotator cuff tendons are generally good candidates for conventional total shoulder replacement. Depending on the condition of the shoulder, your surgeon may replace only the ball. Sometimes, this decision is made in the operating room at the time of the surgery. Some surgeons replace the ball when it is severely fractured and the socket is normal.
Preparation-
Some severe degenerative problems of the shoulder may require replacement of the painful shoulder with an artificial shoulder joint. You and your surgeon should make the decision to proceed with surgery together. You need to understand as much about the procedure as possible. If you have concerns or questions, you should talk to your surgeon.
Once you decide on surgery, you need to take several steps. Your surgeon may suggest a complete physical examination by your regular doctor. This exam helps ensure that you are in the best possible condition to undergo the operation.
You may also need to spend time with the physical or occupational therapist who will be managing your rehabilitation after surgery. This allows you to get a head start on your recovery. One purpose of this pre-operative visit is to record a baseline of information. Your therapist will check your current pain levels, ability to do your activities, and the movement and strength of each shoulder.
A second purpose of the pre-operative visit is to prepare you for surgery. You’ll begin learning some of the exercises you’ll use during your recovery. And your therapist can help you anticipate any special needs or problems you might have at home, once you’re released from the hospital.
On the day of your surgery, you will probably be admitted to the hospital early in the morning. You shouldn’t eat or drink anything after midnight the night before. Come prepared to stay in the hospital for several nights. The length of time you will spend in the hospital depends a lot on you.
What is the Shoulder Replacement Surgery Cost in India?
The Cost of Shoulder Replacement Surgery in India can range from approximately Rs. 4,00,000 ($5,000) to Rs. 5,60,000 ($7,000).
The cost will be depending upon the Stage of Arthritis, Type of Surgery required, Investigation & evaluation required, Specialty of Surgeon, Hospital Fee, and Room Category.
Top 10 Shoulder Replacement Surgery Hospitals in India
- Fortis Hospital, Delhi
- Max Hospital, Delhi
- Artemis Hospital, Delhi
- BLK Hospital, Delhi
- Nanvati Hospital, Mumbai
- Global Hospital, Mumbai
- Manipal Hospital, Bangalore
- Kokilaben Hospital, Mumbai
- Saifee Hospital, Mumbai
- Medanta Hospital, Gurgaon
10 Best Shoulder Replacement Surgeons in India
- Dr. Kaushal Malhan
- Dr. Haresh Mangalani
- Dr. Ashok Rajgopal
- Dr. Aditya Menon
- Dr. Sanjay Sarup
- Dr. IPS Oberio
- Dr. Sachin Bhonsle
- Dr. Harshwardhan Hegde
- Dr. Pradeep B. Bhosale
- Dr. Anil R Karkhanis
Planning Your Affordable Shoulder Replacement Surgery in India is an Easy Process.
Our Hospitals Network and Surgery Group is available in 15 cities of India for our patients to access. Kindly fill up the form for a free opinion from our expert team. You will be provided with an analysis and recommendations for your surgery. NO CHARGES LEVIED.
Special ALL SERVICES INCLUSIVE Packages available for INTERNATIONAL PATIENTS
Operation-
Shoulder replacement surgery can be done in one of two ways. When the cartilage of both the humeral head (the ball) and the glenoid (the socket) is worn away, both parts of the joint must be replaced. This surgery is called arthroplasty, which is the term used for joint reconstruction.
If the glenoid still has some articular cartilage, your surgeon may replace only the humeral head. This procedure is known as a hemiarthroplasty. (Hemi means half.) The hemi-arthroplasty is most commonly used after a fracture of the shoulder where the blood supply to the ball portion (the humeral head) of the humerus is damaged. Research has shown that when the shoulder is being replaced for arthritis, the complete shoulder arthroplasty performs better. Patients have less pain immediately after surgery and in the long run have a better functioning shoulder with less complication and are less likely to need a second operation.
You will most likely need general anesthesia for shoulder replacement surgery. General anesthesia puts you to sleep. It is difficult to numb only the shoulder and arm in a way that makes such a major surgery possible.
Shoulder replacement surgery is done through an incision on the front of your shoulder. This is called an anterior approach. The surgeon cuts through the skin and then isolates the nerves and blood vessels and moves them to the side. The muscles are also moved to the side.
The surgeon enters the shoulder joint itself by cutting into the joint capsule. This allows the surgeon to see the joint.
At this point, the surgeon can prepare the bone for attaching the replacement parts. The ball portion of the humeral head is removed with a bone saw. The hollow inside of the upper numerus is prepared using a rasp. This lets your surgeon mold the space to anchor the metal stem of the humeral component inside the bone.
If the glenoid will be replaced, it is prepared by grinding away any remaining cartilage on the surface. This is done with an instrument called a burr. The surgeon usually uses the burr to drill holes into the bone of the scapula. This is where the stem of the glenoid component is anchored.
Finally, the humeral component and the glenoid component are inserted and the humeral ball is attached.
Once the joint is anchored, the surgeon tests for proper fit. When the surgeon is satisfied with the fit, the joint capsule is stitched together. The muscles are then returned to their correct positions, and the skin is also stitched up.
Your incision will be covered with a bandage, and your arm will be placed in a sling. You will then be woken up and taken to the recovery room.
After surgery-
After surgery, you’ll be transported to the recovery room. You will have a dressing wrapped over your shoulder that will need to be changed frequently over the next few days. Your surgeon may have inserted a small drainage tube into the shoulder joint to help keep extra blood and fluid from building up inside the joint. An intravenous line (IV) will be placed in your arm to give you needed antibiotics and medication.
Your shoulder may be placed in a continuous passive motion (CPM) machine immediately after surgery. CPM helps the shoulder begin to move and alleviates joint stiffness. The machine straps to the shoulder and continuously bends and straightens the joint. This motion is thought to reduce stiffness, ease pain, and keep extra scar tissue from forming inside the joint. You’ll use a shoulder sling to support your arm when you’re not using the CPM machine.
Rehabilitation-
A physical or occupational therapist will see you the day after surgery to begin your rehabilitation program. Therapy treatments will gradually improve the movement in your shoulder. If you are using CPM, your therapist will check the alignment and settings. Your therapist will go over your exercises and make sure you are safe getting in and out of bed and moving about in your room.
When you go home, you may get home therapy visits. By visiting your home, your therapist can check to see that you are safe getting around in your home. Treatments will also be done to help improve your range of motion and strength. In some cases, you may require up to three visits at home before beginning outpatient therapy.
The first few outpatient treatments will focus on controlling pain and swelling. Ice and electrical stimulation treatments may help. Your therapist may also use massage and other types of hands-on treatments to ease muscle spasm and pain. Continue to use your shoulder sling as prescribed.
As the rehabilitation program evolves, more challenging exercises are chosen to safely advance the shoulder’s strength and function.
Finally, a select group of exercises can be used to simulate day-to-day activities, like grooming your hair or getting dressed. Specific exercises may also be chosen to simulate work or hobby demands.
When your shoulder range of motion and strength has improved enough, you’ll be able to gradually get back to normal activities. Ideally, you’ll be able to do almost everything you did before. However, you may need to avoid heavy or repeated shoulder actions.
You may be involved in a progressive rehabilitation program for two to four months after surgery to ensure the best results from your artificial joint. In the first six weeks after surgery, you should expect to see your therapist two to three times a week. At that time, if everything is still going as planned, you may be able to advance to a home program. Then you will only check in with your therapist every few weeks.
Why Choose India for Shoulder Replacement Surgery?
Joint Replacement Surgery Hospital India offers highest quality bone and joint health care with attentiveness, care and compassion to meet the needs of the patients and their loved ones. The medical team includes board-certified orthopedic surgeons who are familiar with all the aspects of the musculoskeletal system. Our hospital uses the most advanced technologies available for the orthopedic procedures and has a lower complication rate.
Since the shoulder replacement surgery is a complex operation, we have an experienced surgical team and fully equipped operation theatre facility with excellent infrastructure for the post-operative care and rehabilitation. The shoulder fracture surgery when performed by a high-volume surgeon under a high-volume hospital provides you a better outcome.
Are you looking for Affordable Cost of Shoulder Replacement Surgery in Top Hospitals of India?
Please enquire with us Get a “No Obligation Quote”
If you are really seeking for Shoulder Replacement Surgery, kindly fill up the form for a free consultation with our surgeons. You will be provided with thorough analysis and suggestions regarding the Shoulder Replacement Surgery you are seeking.
Listen to the Voices of Our Happy Patients
FAQ’s
Arthritis. Arthritis is the result of the cartilage in a joint being worn out over time. I often describe the arthritis in the shoulder as having a “rusty hinge”. The cartilage in your joint is supposed to be a smooth surface that allows things to move easily; however, when the cartilage wears out as a result of arthritis it becomes a rough surface, or “rusty”.
If you have pain in your shoulder, limited function and difficulty sleeping it is important to try arthritis medications and cortisone injections. If the medication and injections do not relieve your shoulder pain, then it is time to discuss a shoulder replacement.
The typical age group for a shoulder replacement patient is 60-80 years old. I have performed shoulder replacements on patients as old as 88 and as young as the mid-40s. Every patient’s situation is uniquely different and I take that into consideration when discussing a shoulder replacement.
For the most part it is not valuable to do therapy or exercise before a shoulder replacement surgery. Unfortunately the movement further aggravates the shoulder and causes more pain. My preparation advice for shoulder replacement surgery is more focused on the practical things in life… you have to prepare for the fact that you aren’t going to have use of your arm for a matter of weeks, which means you might need some help at home (cooking, showering, driving, etc.). I don’t recommend you drive for at least a couple of weeks following surgery. It is important for patients to plan ahead and understand what the nuts/bolts are regarding their recovery.
Certain foods, more related to nutritional supplements, can cause your blood to be thinned, a similar effect as aspirin or blood thinners. I will go over a list of supplements that could have this effect… I will have you stop taking those items a week prior to your shoulder replacement surgery.
There is some immediate change in regard to the movement of the shoulder being much smoother; however, for a few weeks after surgery it is more painful than before surgery. At about two weeks post-surgery people start to get over the “hump” and it is less painful than prior to surgery. The pain will continue to gradually decrease. At two months the average patient is very happy they had their shoulder replaced.
Most people require, to some degree, oxycodone or hydrocodone. In addition, I supplement anti-inflammatory medications. Each patient is very unique and their pain levels vary, naturally I make those adjustments accordingly.
The first couple of days the pain will be significant, but it can also be controlled with the appropriate medications. Regaining range of motion takes time, patience and persistence it only improves at a certain rate each month.
Yes. The typical stay is somewhere between 24-48 hours: 50% stay one day while 50% stay two days. Rarely do patients stay longer than two days.
Yes, we will prescribe physical therapy. Typically, therapy will last two months following the operation; however, sometimes patients require more.
Most people who develop arthritis on one side develop it on the other side as well. Most often one side hurts worse than the other and so many patients opt for both shoulders to be replaced, but it is usually a couple years between the two operations.
The estimate is around 15 years, but that estimate is variable and we see them last longer in some patients. It is difficult to predict how long each patient’s shoulder replacement will last, specifically because the materials we use now are improved from those 7-8 years ago.
Typically, if you need a shoulder redone, you redo the whole thing (not just parts), but it is rare that we have to do that. For most people, their shoulder will last for as long as they need it; however, that depends on the age that the patient received their replacement.
Infection is always the number one concern. We take a lot of precaution to prevent an infection when it comes to the surgery technique and antibiotics (you get antibiotics around the time of surgery). There is a possibility I can injure a very important nerve in the shoulder that is close to where I am working. If that nerve is injured it can have an impact on your ability to raise your arm above your head. I am very mindful of that nerve during the surgery. From a practical standpoint, wear and tear of the parts over time can cause complications.
Construction worker: 3 months
Desk worker: 2 weeks
Almost everyone has a thorough physical exam with their primary care physician to make sure they are healthy enough to handle the stress of replacement surgery. In addition, the biggest thing to plan for is to have help at home. We also don’t recommend you drive for at least a couple of weeks following surgery.






 English
English Arabic
Arabic French
French Bangla
Bangla Russian
Russian